Achilles tendon pain is one of the most common sites of dysfunction in recreational and elite athletes. It is also relatively common in the sedentary population too. Studies of tendons have shown that changes occur within the tendon itself and it has been suggested that exercise or loading of the tendon is possibly just something that provokes a symptomatic change rather than being the cause of the pathology. In other words, we all incur tendon changes over time, just some of us become symptomatic!
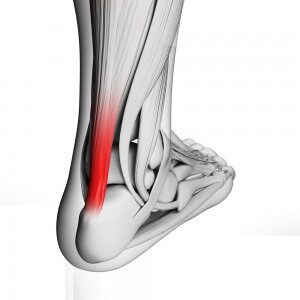
So, establishing why one person becomes symptomatic and another does requires careful consideration. Common factors are thought to be biomechanics, footwear, changes in routine, sudden increases in training / loading, poor strength and stability from above the foot and ankle.
As mentioned already, studies that have looked into the health and make-up of dysfunctional achilles tendons have found numerous significant changes to the tendon matrix. The main changes are centred around the body’s attempt at healing the tendon – a process that isn’t always as successful as we might expect.
Firstly, an increase in cell activation and the total number of cells occurs. This gives rise to the classic thickened feel of a chronic Achilles tendinopathy. There is also an increase in the ground substance – a non fibrous gel-like substance that sits around the dysfunctional tendon.
Secondly, collagen fibres, the building blocks of a tendon, are usually arranged in a longitudinal fashion. In the case of an Achilles tendinopathy they become misaligned and instead are arranged in a random order – creating a weakened structure no longer fit for purpose. The type of collagen fibre (type 3) that is found in dysfunctional tendons is also a weaker version of the stronger type 1 & 2 fibres found in healthy tendons. These type 3 collagen fibres are favoured by collagen producing cells called tenocytes due to the changes in the chemical make up of a painful tendon.
Lastly and arguably the most significant in terms of the cause of pain is a phenomenon called neo-vascularisation. This is the growth of tiny new blood vessels into the tendon. Alongside these new blood vessels grows new nerves and it is these that give rise to the pain. The other significant cause of pain is thought to be chemical pain. One study has shown that natural neurotransmitter chemicals (modulating pain sensations in the nervous system) are found in greater numbers in dysfunctional tendons when compared to non-painful tendons.
Contrary to popular belief, research has shown that there is little (if any) inflammation of the tendon itself. However, there is a sheath that surrounds the tendon and this sheath can often become irritated and therefore inflamed by the thickened, chemical rich tendon within its walls.
So, that covers (in a nutshell) how and why a tendon can become painful and dysfunctional but does not answer the question on everybody’s lips: how do we fix a dysfunctional Achilles tendon?
Once the cause or likely causative factors have been established, a management plan can be formed. Extrinsic factors to consider adapting are along the lines of activity modification and equipment adjustment. Intrinsic factors might include treatment of any local inflammation of the tendon sheath (if present), pain control with medication or treatment techniques, soft tissue treatment to address areas of tension / tightness, biomechanical correction, strengthening exercises and most importantly, loading the tendon in a specific way.
Most recent studies show the best way to load the tendon in rehab is to perform eccentric exercises. This is where the tendon is worked as the muscle unit is lengthened. The most common way to do these exercises is to stand on the edge of a step and lower your heel down slowly. There is some debate in the scientific literature as to the optimum number and frequency of these exercises but the benefits are clear to see. The effect of this eccentric loading at a cellular level basically helps to make the type of collagen (building blocks of tendon fibres) more suited to the load by creating more of the stronger type 1 and type 2 collagen fibres and aids reorganisation of these fibres. Some of the other effects that have been suggested to take place are a shearing of the new blood vessels and associated nerve endings within the tendon as well as altering fluid transfer and chemical make up within the tendon. In summary, the end result is a stronger, healthier tendon, which is better able to withstand load and less likely to cause pain.
The simplistic view would be to say everyone who has Achilles tendon dysfunction and pain, should perform eccentric exercises. However, we have established that Achilles tendinopathies are a multi-faceted problem and require careful thought with regards to establishing a cause, treating this to prevent recurrence and then loading the tendon appropriately to be able to cope with functional demands of the specific athlete or patient.
If you are suffering with Achilles tendon pain, contact Fit4-Physio for a detailed assessment and suitable treatment plan – why be in pain when you could perform!

